|
See link below under Related Letters for Texas Board of Nursing Response or click here
April 20, 2013
Katherine A. Thomas, MN, RN, FAAN
Executive Director
Texas Board of Nursing
333 Guadalupe #3-460
Austin, Texas 78701
kathy.thomas@bne.texas.gov
Dear Ms. Thomas:
As the Chief Executive Officer of a medium size multi-specialty practice in Beaumont, Texas, I am requesting clarification by the Texas Nursing Board of the scope of practice for registered nurses (RNs). The origin of this inquiry is a meeting held by Christus St. Elizabeth administrative staff with the assistance of consultant. Baptist Hospital of Southeast Texas had a similar meeting in January. The purpose of these meetings is to limit the scope of practice by RNs who are credentialed by the hospital and who are employed by physicians to work in the hospital.
Index to Content
Introducing SETMA
The Issue Raised in the Hospital Meeting
The Context and Development of RNs working for Physicians in the hospital
The Contradictions between healthcare Reform, Innovation and Regulations
The Innovator’s Prescription: A Disruptive Solution for Health Care
SETMA’s Team Approach
The impact of Electronic Medical Records (EMR) on the relationships between various members of the healthcare team
The Future
Current RN Scope of Practice - Texas Nursing Board
What SETMA is asking of the Texas Nursing Board
Plan of Action
SETMA’s Care Coordination Department
As an NCQA tier three recognized medical home, we are currently reapplying for recognition as we are completing our first three-years as a PC-MH. SETMA is also an AAAHC credentialed medical home and ambulatory care center. We are a Diabetes Center of Excellence. SETMA employees a hospital-care team which includes RNs and CFNPs and a clinic staff of 13 CNFPS and multiple RNs, LVNs and Nurse Aids. While all of our staff operates within their licensure and skill set, they all are knowledgeable beyond their formal training because of internal quality improvement and continuous professional development.
We are currently participating in a Robert Wood Johnson Foundation (RWJF) three-year study of SETMA. RWJF designed a research project, “At a time when a shortage of primary care providers is threatening the accessibility and quality of care in the country, the RWJF is teaming with the Group Health Research Institute on a new national program designed to identify creative practices that make primary care more efficient and effective. The Primary Care Team: Learning from Effective Ambulatory Practices (the LEAP Project) will identify primary care practices that use health professionals and other staff in ways that maximize access to their services, so these workforce models can be replicated and adopted more widely.”
The following is a link to the 59-page report SETMA submitted to RWJF before we were selected for the study. The Primary Care Team: Learning from Effective Ambulatory Practices (PCT-LEAP): Performance Measures Worksheet - Robert Wood Johnson Foundation.
We are also involved with a research project with the American Board of Family Medicine and with the Johnson and Johnson Corporation. At www.jameslhollymd.com under Public Reporting, SETMA reports on over 300 quality metrics by provider name. Data is reported for 2009, 2010, 2011, 2012 and the first quarter of 2013. Below is an example of reporting on the metrics for NCQA Diabetes Recognition with the performance of nurse practitioners outlined in red:
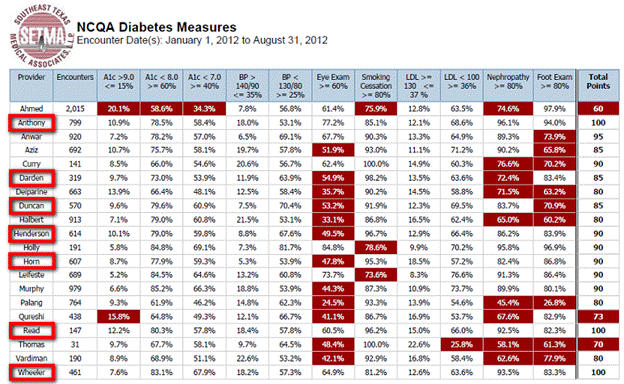
In recent audits by the Center for Medicare and Medicaid Services (CMS) concern was raised that RNs and in at least one case an Licensed Vocational Nurses (LVN) have been operating outside of their scope of practice in the:
- Completion of hospital admission history
- Issuing of treatment orders for hospital inpatients
- Completion of discharge summaries from the hospital
While this discussion probably applies to almost all primary care practices employment of RNs and Certified Family Nurse Practitioners (CFNP) in the hospital, I can only attest to the practice of Southeast Texas Medical Associates, LLP (SETMA. www.jameslhollymd.com)
In the 1970s, specialists, particularly cardiologists, began employing RNs to improve the transitions of care from the hospital. The RNs completed medication lists, which were handwritten with directions for use and with explanations for why the medications were being prescribed. Gradually, these RNs began completing initial patient evacuations and daily progress notes and discharge planning and instructions.
As is still the case, no charges were submitted to CMS or to other insurance companies for the work of these RNs. They were trained by the specialists and treatment guidelines were established for excellence of care and for patient safety. As long as this process was practice by the specialists no objection was raised.
Gradually, as the demand upon primary care increased and as the complexity of care increased more and more primary care physicians employed RNs in similar capacities. Again, no charges to CMS or other insurance companies were generated for the work of these nurses. The nurses’ work accomplished:
- Improving of care as to continuity, quality and immediacy
- Improving of the quality of life of the healthcare providers as their sharing of responsibly of care allowed for excellence of care and proper rest for the providers.
Effective collaboration between members of the healthcare team has been a hallmark of healthcare innovation, particularly in regard to patient-centered medical home. Physicians and nurses have increasingly become colleagues rather then employer/employee.
There is an increasing public policy pressure to expand the RN scope of practice while protecting public safety but there is also increasing bureaucratic pressure which is resisting this change because it does not fit our current model of care. No where is this conflict more clearly addressed than in The Innovator’s Prescription: A Disruptive Solution for Health Careby Clayton M. Christensen.
The following excerpts from that book help clarify the problem we are trying to address.
“Levels of medicine
- “When precise diagnoses aren’t possible...intuitive medicine, where highly trained and expensive professionals solve medical problems through intuitive experimentation and pattern recognition.” (XXII) (emphasis in original)
- “As patterns become clearer, care evolves into the realm of evidence-based medicine, or empirical medicine - where data are amassed to show that certain ways of treating patients are, on average, better than others.” (XXII) (emphasis in original)
- “Only when diseases are diagnosed precisely...can therapy that is predictably effective ...be developed and standardized. We term this domain precision medicine.” (XXII) (emphasis in original)
“Change wrought by Precision Medicine
- “...(when) we know what type of bacterium, virus, or parasite causes one of these disease...
- “...(when) we know the mechanism by which the infection propagates...
- “...predictably effective therapies can be developed...
- ...therapies that address the cause, not just the symptoms...” (XXIII)
“As a result
- “....nurses can now provide care for many infectious diseases...
- “...patients with these diseases only rarely require hospitalizations.” (XXIII)
“II. Disruptive Business Model Innovations
- “...many technological enablers have not...been translated into lower-cost, higher-quality more accessible services...why...” (XXIII)
- “...delivery of care has been frozen in...general hospital and the physician’s practices - both...designed a century ago...in the realm of intuitive medicine.” (XXIII)
- “...lack of business model innovation...in many cases because regulators have not permitted it...” (emphasis added)
The current tension between medical practice, hospital administrators, CMS and the Texas Nursing Board is a perfect example of “a business model innovation” which has improved care, working effectively toward the Triple Aim, which is not being challenged because “regulators have not permitted it.”
SETMA’s Team Approach
SETMA’s team approach to inpatient care is a success as demonstrated by the facts that our lengths of stay, quality metrics, cost of care and patient satisfaction are excellent. And, it is one of the reasons why the indigent, uninsured and unassigned patients for whom we care receive the same quality of care as our private patients. I would offer the following observations about SETMA’s team. SETMA has licensed and credentialed healthcare professionals who work to the top of, but not beyond their legal scope of practice as defined by each of their accreditation agencies.. As a policy issue, the prestigious and influential Health Affairs of January 14, 2013, published an extensive article entitled, Primary Care Physician Shortages Could Be Eliminated Through Use Of Teams, Non-physicians, And Electronic Communication. The goal of this transformation is to integrate teams to increase their efficiency, excellence and economy. This is what SETMA started eighteen years ago.
There is resistance to this transformation. In September 2010, the Texas Higher Education Coordinating Board was considering allowing two Texas Health Science Centers’ Schools of Nursing to expand their programs to offer the Doctor of Nurse Practitioner degree. It is hard to believe but one physician member of that board testified that nurses should be giving enemas and using bedpans rather than getting doctoral degrees. I wrote the coordinating board and said:
“Most physicians have not had the opportunities which I have in order to appreciate the value of the nurse practitioners role and now the doctor of nurse practitioner role. In an article for my weekly column for October 21.m 2009 entitled, Re-Evaluating the Value of Members of the Healthcare Team, I said:
‘It is easily recognized in this emerging paradigm that all of the schools in the academic healthcare center are actively involved in patient care and in the training of those who will be healthcare providers. Yet, it seems that the farther and farther a person advances in biomedical education, the obvious union of their disciplines at their foundations seems to be lost and the more isolated from the whole these ‘specialists’ and ‘experts” become.
‘This even creates problems within the various disciplines as egocentrism isolates one medical specialty from another. It is as a result of the need for the integration of healthcare disciplines at the delivery level, that the imperative becomes obvious for the restructuring of the training of the members of this healthcare team.
‘And, the first change must come in the relationships between the leaders of the training programs who educate and mentor future healthcare scientist, teachers, caregivers and researchers. The educational leaders must model this integration for their disparate student bodies and that modeling will require the investment of the most precious and rare resource: time.”
The following are three articles SETMA has published that are relevant to the role of RNs in the innovative transformation of healthcare.
- Article 3 is from 2010 and addresses the need for integrating the education and training of components of the healthcare team.
- Article 2 is from January, 2013 and is an analysis of SETMA inpatient team care. This article is the most directly relevant to scope of practice.
- Article 1 is a look at the future of team collaboration and a response to the criticism of the CMS rules on RN participation on the healthcare team.
- The Future of Collaboration Between Physicians and Nurses
- SETMA's Inpatient Team Based Process Analysis: The Interaction of SETMA’s Hospital Care Team - Collegiality and "Electronic Huddles"
- Re-Evaluating the Value of Members of the Healthcare Team
In October, 2010, I wrote:
“The ideal setting in which to deliver and to receive healthcare is one in which all healthcare providers value the participation by all other members of the healthcare-delivery team. In fact, that is the imperative of Medical Home. Without an active team with team consciousness and team collegiality, Medical Home is just a name which is imposed upon the current means of caring for the needs of others. And, as we have seen in the past, the lack of a team approach at every level and in every department of medicine creates inefficiency, increased cost, potential for errors and it actually eviscerates the potential strength of the healthcare system.
“Why is this? Typically, it is because healthcare providers in one discipline are trained in isolation from healthcare providers of a different discipline. Oh, they are in the same buildings and often are seeing the same patients but they rarely interact. Even their medical record documentation is often done in compartmentalized paper records, which are rarely reviewed by anyone but members of their own discipline. This is where the first benefit of technology can help resolve some of this dysfunction. Electronic health records (EHR), or electronic medical records (EMR) help because everyone uses a common data base which is being built by every other member of the team regardless of discipline. While the use of EMR is not universal in academic medical centers, the growth of its use will enable the design and function of records to be more interactive between the various schools of the academic center.
“And, why is that important? Principally, because more and more healthcare professionals are discovering that while their training often isolates them from other healthcare professionals, the science of their disciplines is crying for integration and communication. For instance, there was a time when physicians rarely gave much attention to the dental care of their patients, unless they had the most egregious deterioration of teeth. Today, however, in a growing number of clinical situations, such as the care of diabetes, physicians are inquiring as to whether the patient is receiving routine dental care as evidence-based medicine is indicating that the control of disease and the well-being of patients with diabetes are improved by routine dental care. Also, as the science of medicine is proving that more and more heart disease may have an infectious component, or even causation, the avoidance of gingivitis and periodontal disease have become of concern to physicians as well as dentist.”
It is my hope that the Texas Nursing Board, CMS and hospital administrators do not push back the clock and return us to the healthcare silos where teams did not exist, care was fragmented and patient safety suffered from both.
| The impact of Electronic Medical Records (EMR) on the relationships between various members of the healthcare team | Index |
Most of the resistance t changing roles in health stemmed from a time when every patient encounter was a de novo event. Patient records where encased in paper records which were available in only one place and there was no continuity from one episode to another.
Fundamental
Fundamental to this entire discussion is the “change of mind” which healthcare providers and surveyors must have. This metanoia (change of mind) must take place in order for surveyors to distinguish between the excellence of the new and the excesses and abuses of the past, which may at first glance seem similar. They must know that SETMA’s patients are not treated in isolation, as patients have traditionally been treated. Traditionally, medical records were locked up in the providers’ offices, or in the hospital’s medical records department. To judge SETMA by the state of care given by healthcare providers who do not have an integrated delivery system with robust electronic patient management is to do a disservice to all of us.
In the emergency department (ED) and in the hospital, traditionally, the only data continuity was provided by the availability of old hospital admission records. The problem with those records is that there may by several years of time and dozens of visits and modifications of the patient’s treatment plan, since the last hospitalization. So, at best the available records were incomplete and at worst were so outdated they were useless. And, even when those records were available, they were not interactive. Information had to be extracted from the old record and entered into the new record. And as mentioned, if the patient had been seen, evaluated and treated fifteen times since the last hospitalization, none of those treatment events was available.
Not so, with SETMA. Every encounter, hospital, ED, clinic, all SETMA clinics, physical therapy, etc., is available to the provider who is assessing the patient. All of SETMA’s patients’ records are instantly available where ever our patients are being treated and particularly in the emergency department and in the hospital in-patient setting. That means that there is continuity of care between the ambulatory setting and the ED and inpatient settings, based on the documentation of the patient’s health care in the past. Medications, diagnoses, treatment plans and plans of care, laboratory data, and physician plans and consultations notes are all instantly available.
Rarely is a SETMA patient seen in the ED or hospital where the patient has not already had an exhaustive and established diagnoses and plan of care in the clinic. In addition, the EMR has 29 sets of guidelines for care and each patient has a physician-determined treatment plan in the EMR which plans are easily accessed by any and all SETMA providers. When the ER physician diagnoses CHF, SETMA has a treatment plan already written for the excellent and expert treatment of CHF. This is true of COPD, Pneumonia, Respiratory Failure, etc. Even the treatment orders, which are based on a physician’s diagnoses, are produced by electronic algorithms which are vetted by experts and embedded in our EMR.
For those patients who are new to SETMA, the diagnostic assessment and the treatment plan is initially determined by the ED physician and not by SETMA’s RN. There is always a SETMA physician available and typically one is in the hospital until 8 or 10 PM and others come in to the hospital between 2 and 4 AM, leaving only 4 to 8 hours a day when a SETMA physician is not physically available for patient care and collaboration with the SETMA nursing staff either in a personal “huddle” or in an “electronic huddle” by telephone or secure e-mail..
Electronic Huddles
One of the elements of Patient-Centered Medical Home is a “huddle.” where a team of providers meet daily to discuss a patient’s care. SETMA is introducing the world to “electronic huddles” made up of multiple communications daily:
- Morning notes electronically generated and submitted to the hospital care team daily. These notes give guidance to SETMA’s staff who work in the hospital around the clock to provide continuity of care and quality care to all of SETMA’s patients.
- iPhone contacts repeatedly during the day and night. The ability for nursing staff to communicate detailed notes, procedure results or x-ray and lab reports, adds to the continuity of care and to the rapidity with which information is communicated to the entire healthcare team.
- Secure e-mail allows procedure and test results to be communicated to the provider by the hospital staff allowing adjustments to treatment and initiation of new treatments to occur continuously all day and night.
- Electronic consultations with consultants and/or specialists can be done efficiently and timely.
Rather than a single point of care once a day, SETMA’s patients receive multiple points of care, multiple times a day, all initiated by physicians and all carried out by members of SETMA’s team. SETMA’s Model of Care has more physicians and more team member interacting on more patients every day than in any other model. The reality is that with multiple “sets of eyes” on a patient’s care, patient safety goes up as it is not unusual for experienced and knowledgeable RNs to bring an issue to the physicians’ attention which has not been addressed. The physician then gives instructions as how to respond but the real credit belongs to the nurse. This is only one example as to how the team increases the patient’s quality of and safety of care. RNs are not being asked or even allowed to operate outside of their licensure, but they are a dynamic and essential part of the healthcare delivery team..
On admission, after the history and physician examination is reviewed and approved by the physician, every patient admitted to SETMA receives a Hospital Plan of Care, which is a printed, personalized record of the patient’s diagnoses, consultations, procedures, tests, how long the patient is expected to be in the hospital, the probability of readmission upon discharge, a reconciled medication list and a precise explanation of how to contact both the admitting and attending physician and SETMA’s hospital support time This is in keeping with the PC-MH Model where our “electronic huddles” even involve the patients and their family.
Discharge Summaries, now called Hospital Care Summary and Post Hospital Plan of care and Treatment Plan
As for the discharge summary, that is a function of the chart notes, discharge instructions written by the physician and the morning electronic “huddle,” where a summary is sent to the hospital care team. Incidentally, if needed, SETMA can produce those documents for the past eight years. Remember, we don’t do discharge summaries; we do “Hospital Care Summaries and Post Hospital Plans of Care and Treatment Plans” which are produced from the entire written record, “electronic huddles,” oral communications, but NOT from RNs acting independently of healthcare providers.
This is a brief summary of SETMA’s team approach. We believe this exceeds the current standard of care in our community. The accreditation visit has given us the opportunity to think about what we are doing. And, as is our nature, we will continue to improve the process as a result.
Increasingly, the superior efficiency, excellence and safety of team-based care is being recognized. As with electronic health records and with electronic patient management, these changes are challenging to old ways of thinking about healthcare and with old ways of doing “healthcare.” Yet, if we wish to fulfill the Triple Aim as enunciated by the Institute for Healthcare Improvement (IHI) in 2007, we must change. If we are going to improve care (a process), health (an outcome) and at the same time decrease the cost of care (sustainability), we must be committed to evidence-based medicine, to electronic patient management, to a team organized around a Patient-Centered Medical Home and to a new method of payment similar to capitation with payment for quality as seen in Medicare Advantage programs.
| Current RN Scope of Practice - Texas Nursing Board | Index |
| What SETMA is asking of the Texas Nursing Board? | Index |
As I read the Texas Nursing Practice Act and the official, board-endorsed Position Statements which expand the description of the RN Scope of Practice, there are many questions not addressed clearly. The position statements on RNs carrying out order from CFNPs and PAs are helpful. It would be very helpful if the Board spoke officially on hospital staff nurses ability to receive orders from a hospital-credentialed RN who is employed by a physician when that order originates with an physician who is on he staff of the hospital.
The following is the Texas NPA’s description of the RN’s Scope of Practice:
“The professional registered nurse is an advocate for the patient and the patient’s family, and promotes safety by practicing within the NPA and the BON Rules and Regulations. The RN provides nursing services that require substantial specialized judgment and skill. The planning and delivery of professional nursing care is based on knowledge and application of the principles of biological, physical and social science as acquired by a completed course of study in an approved school of professional nursing. Unless licensed as an advanced practice registered nurse, the RN scope of practice does not include acts of medical diagnosis or the prescription of therapeutic or corrective measures.2 RNs utilize the nursing process to establish the plan of care in which nursing services are delivered to patients. The level and impact of the nursing process differs between the RN and LVN as well as between the different levels of RN education (see Table).” (emphasis added)
I have also studied the Six-Step Decision-Making Model for Determining Nursing Scope of Practice and can find nothing which indicates that our deployment of RNs on our team violates any element of the TNA.
- The verbal transition of an order from a physician via an RN to a hospital-staff RN does not represent an “act of medical diagnosis or a prescription of therapeutic or corrective measure” by an RN.
- Because we are now working in an environment at SETMA where the continuum of care patient record is available at ALL points of care, the RN’s placement of the diagnoses and plan of care and orders into a formal electronic document based on documentation by a SETMA or an ER physician’s assessment and instructions, does not represent the “medical diagnosis or prescription of therapeutic or corrective measures.”
- And, because the Hospital Care Summary and the Post Hospital Plan of Care and Treatment Plan (previously called the “Discharge Summary”) is a product of the hospital record and of verbal and electronic huddles between the RN and the treating physician, this does not represent “medical diagnosis or prescription of therapeutic or correction measures” by the RN.
I am going to be speaking at the Test Texas HIV Coalition Meeting May 3, 2013, I request to be able to speak to you in person and to other members of the TNB you would recommend on May 2, 1013. After a careful review of SETMA’s work, I would like to ask you to issue a Board assessment that SETMA is working within in the RN’s Scope of Practice and to communicate that assessment to CMS and to the administrations of Christus St. Elizabeth in Beaumont and to Baptist Hospital of Southeast Texas.
Furthermore, at SETMA’s expense, I would like to invite you and any other members of your staff you would designate to visit SETMA and to allow us to introduce you to our team-based, patient-centered medical home approach to healthcare.
Thank you for reading this appeal. This is an important matter. The future of healthcare transformation is at stake.
James (Larry) Holly, M.D.
C.E.O. SETMA
www.jameslhollymd.com
(409) 504-4517
Adjunct Professor
Family & Community Medicine
University of Texas Health Science Center
San Antonio School of Medicine
Clinical Associate Professor
Department of Internal Medicine
School of Medicine
Texas A&M Health Science Center
Few of SETMA’s activities address our transformative and innovative efforts as does our Care Coordination Department. The following is a summary of that Department’s work as of January, 2013. While this does not directly affect our appeal for modifications in the Texas Nursing Act or in the RNs’ Scope of Practice, it does help define the organization which is making this appeal.
Formed as an integral part of SETMA’s Patient-Centered Medical Home, the Department currently consists of four full-time staff members including the Director, a Care Coordination Technician, Registered Nurse and Licensed Vocation Nurse.
This department began its work in August, 2010. At that time, there were two nurses that made calls to patients that were discharged from the hospital. Simultaneously with the creation of the Department, and after attending a Care Transitions Workshop at the National Quality Forum, the traditional Hospital Discharge Summary was renamed to Hospital Care Summary and Post Hospital Plan of Care and Treatment Plan. This longer but more functional name became the hub of SETMA’s Care Transition and established a seamless continuity of care between the inpatient and ambulatory care settings. It also became the laboratory in which other tools were developed in order to make sure that better care (a process) resulted in better health (an outcome). One of those is that upon admission to the hospital, each patient receives a Hospital Plan of Care, which tells them why they are being admitted, how long they should expect to stay, their risk of readmissions after being discharged, their medications, procedures, tests, etc.
Pursuing the goals of the Institute for Healthcare Improvement’s (IHI) Triple Aim, NCQA PC-MH, AAAHC Medical Home, and SETMA’s goal of decreasing avoidable readmissions, a new function was added to the Hospital Care Summary and Post Hospital Plan of Care and Treatment Plan: the Hospital Follow-up Telephone Call and the Clinic Follow-up Telephone Call. All patients discharged from the hospital receive a telephone call which lasts from twelve to thirty minutes. (With the frail elderly, the telephone call can last for two hours.) Following a clinic visit, when a patient’s care is complex and adherence is critical, a function was established to enable a note to be sent from the healthcare provider in the clinic to the care coordination department, This allows for a follow-up call to be placed to the patient at the provider’s discretion. SETMA’s tutorial for the use of these follow-up-telephone functions can be reviewed at Using the Clinic and Hospital Follow-up Call Templates.
Care Coordination Department Role
At this review (01.08.13), the department completes on average 2500 outgoing calls per month (30,000 per year). This number does not include incoming calls for patient complaints, requests for assistance from the SETMA Foundation, or calls from patients that use the department for “information”.
The Care Coordination Department exists to assist patients in accessing the care which has been prescribed by SETMA providers, to assist patients with their recovery from a hospital stay, and to help insure that all their medical needs are being met to the best of SETMA’s ability. The care coordination department also expedites care when a referral or a delay would decrease the quality of the patient’s care. This is particularly the case when the patient states they cannot keep their appointment for lack of transportation. Care Coordination can almost always get transportation arrange quickly. A portion of each call to patients after hospital or clinic discharge is utilized in patient education regarding medications, symptoms they may be experiencing and the disease processes with which they are dealing.
Passing the Baton
The Department’s involvement with patient education during the hospital and clinic follow-up calls, enable SETMA to “pass the baton” to the patient so that the patient can be involved in their own care with the caveat that we are always available by phone or secure web portal, if assistance is needed. Our goals are to make certain that patients are accessing the care agreed to with their provider and to enable them to benefit from that care.
The following is the template from which the Hospital Discharge Follow-up Call is communicated from the Hospital Care Team to the Care Coordination Department.
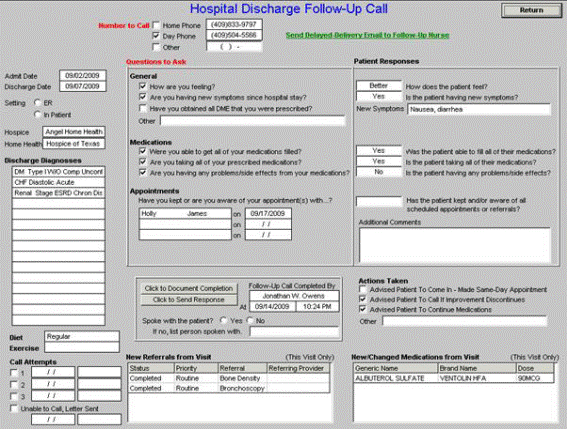
SETMA is committed to making certain that our patients have access to care prescribed and that they can also afford that care. As a result, SETMA’s partners formed The SETMA Foundation through which care can be obtained for our patients which are uninsured, or who cannot afford co-pays, medications, etc. To this end, the partners of SETMA have contributed $2,000,000 to the SETMA Foundation in the past four years.
The Baton
“The Baton” is a pictorial representation of the patient’s “plan of care and treatment plan,” which is the instrument through which responsibility for a patient’s health care is transferred to the patient. Framed copies of “The Baton” hang in all public areas in SETMA’s five clinics and a poster of “The Baton” hangs in over 130 examination rooms. Often, it is forgotten that the member of the healthcare delivery team who carries the ‘baton’ for the majority of the time is the patient and/or the family member who is the principal caregiver. If the ‘baton’ is not effectively transferred to the patient or caregiver, then the patient’s care will suffer.
While healthcare provider performance is important for excellent care of a patient’s health, there are 8,760 hours in a year. A patient who receives an enormous amount of care in a year is in a provider’s office or under the provider’s direct care less than 60 hours a year. This makes it clear that the patient is responsible for the overwhelming amount of their own care which includes adherence with formal healthcare initiatives and with lifestyle choices which support their health.

The poster declares:
Firmly in the providers hand
--The baton - the care and treatment plan
Must be confidently and securely grasped by the patient,
If change is to make a difference
8,760 hours a year.
The poster illustrates:
- That the healthcare-team relationship, which exists between the patient and the healthcare provider, is key to the success of the outcome of quality healthcare.
- That the plan of care and treatment plan, the “baton,” is the engine through which the knowledge and power of the healthcare team is transmitted and sustained.
- That the means of transfer of the “baton” which has been developed by the healthcare team is a coordinated effort between the provider and the patient.
- That typically the healthcare provider knows and understands the patient’s healthcare plan of care and the treatment plan, but that without its transfer to the patient, the provider’s knowledge is useless to the patient.
- That the imperative for the plan - the “baton” - is that it be transferred from the provider to the patient, if change in the life of the patient is going to make a difference in the patient’s health.
- That this transfer requires that the patient “grasps” the “baton,” i.e., that the patient accepts, receives, understands and comprehends the plan, and that the patient is equipped and empowered to carry out the plan successfully.
- That the patient knows that of the 8,760 hours in the year, he/she will be responsible for “carrying the baton,” longer and better than any other member of the healthcare team.
The genius and the promise of the Patient-Centered Medical Home are symbolized by the “baton.” Its display will continually remind the provider and will inform the patient, that to be successful, the patient’s care must be coordinated, which must result in coordinated care. SETMA knows that coordination begins at the points of “transitions of care,” and that the work of the healthcare team - patient and provider - is that together they evaluate, define and execute that care.
Care Coordination attempts to find resources in the community to assist patients, as well assisting them in accessing government programs available. In addition, with the SETMA Foundation, SETMA is able to assist patients with financial needs presented by their medical problems (i.e., co-pays for medications and procedures needed, dental services, transportation costs.). At times, we are working to meet the patient needs in all areas of their lives, including being a “social services” department, making us a well-rounded care coordination department.
The Universal Joint
If the Baton is the tool of care transitions - uniting and sustaining care from one venue to another -- the care coordination department is like a “universal joint” - transferring the power of the healthcare engine to the patient - making it possible to access and apply the care which is prescribed. In the automobile, the power created by the internal combustion engine is transferred to the axles and subsequently to the wheels by the “universal joint.” Without the joint, the powerful engine can run and the high quality wheels and tires can support the vehicle, but the car will not go anywhere.
The same is true of the high powered, evidenced-based medicine which is prescribed by excellent providers. No matter how outstanding the provider is; no matter how accurate the diagnosis is or how correct the treatment is, without the transferring of the knowledge and skills to the patient, nothing will happen. Care Coordination, whether in education, explanation, scheduling, organizing, communicating, makes it possible for patients to access the care they need.
SETMA’s Care Coordination Department
At its founding, the Department had five functions. The following are a list of “duties” performed by the Care Coordination Department at the beginning of 2013. Keep in mind that we encounter many other patient needs which are taken care of as they arise. These needs do not always fall into one of the following categories. :
- Hospital follow-up calls the day after hospital discharge for every patient. At the time of the call, the staff also does an assessment for any barriers the patient may have to their medical care. A third medication reconciliation is done at that time also. The first was on admission, the second was at discharge and the fourth will be at the follow-up clinic visit.
- On Fridays, patients that are in the Care Coordination Department’s workflow before 11:30am, showing that they are being discharged that day, are contacted by phone and information is given on how to contact the SETMA provider on call for afterhours and through the weekend. Patients are encouraged to contact the provider before simply returning to the emergency department.
- Clinic follow-up calls for patients that are at high-risk for readmission to the hospital or who have complex treatment needs, are scheduled by this department after the initial follow-up call. These calls are made to the at-risk patient three days after the initial call, or in the case of a patient that sees the provider on the third day after discharge, the patient is contacted the next day.
- Follow-up calls to patients that miss a hospital follow-up appointment. A report is generated to this department at 8:30am daily and these calls are priority. If we are able to contact the patient, we try to reschedule a same day appointment if at all possible. Also at this time, the staff does an assessment for any barriers the patient may have to accessing the medical care needed.
- Follow-up calls to patients with HTN or DM that miss a scheduled appointment with their provider. Also assessing any barriers the patient may have to receiving the medical care needed.
- For patients with Next MD (SETMA’s secure web portal) accounts and upcoming visits, pre-visit information is sent via this account, as well as those keeping their appointment receive post visit documents from the visit to their electronic account.
- Follow-up calls to all patients that have three or more referrals at one time. Barriers to completion of referrals are discussed and attempts to schedule all referrals on the same day are made. The patient is asked if they are in agreement with the treatment plan. If there are transportation issues, co-pay issues or scheduling issues, the department works to resolve those.
- Infectious disease reporting. Patient demographics and documentation regarding the disease (chart notes, lab work) are faxed to the Beaumont Health Department’s epidemiology nurse. SETMA’s EMR has an electronic tool built which identifies all 87 reportable conditions. When the provider establishes one of those diagnoses an e-mail is automatically sent to Care Coordination which then reports the condition to the State Department of Health. This is per the state protocol - reporting to the region with the region compiling data and then reporting to the state.
- All patient complaint calls. The Department researches the facts about complaints, communicates that to the provider and a response is given. Every effort is made to resolve the issues. Complaints are documented and sent to the Director of Operations and the supervisor of the area where the complaint originated.
- SETMA Foundation assistance. Patients in need are contacted and information is sent to the SETMA Foundation for approval. All arrangements for needed care are handled through this office if assistance is approved by the Foundation.
- The Department also arranges assistance through community programs as needed (Meals on Wheels, Transportation for Seniors, Adult and Child Protective Services, when appropriate, etc).
|